Human Body Systems
The circulatory system consists of a pump (heart), blood (medium) and the blood vessels (channels). There are two types of circulatory system: Open and Closed.
The Open circulatory system consists of a heart and several open ended blood vessels. It is effective in small animals like insects.
The Closed circulatory system consists of the heart, blood and vessels that enclose the blood and allow effective transport of the blood based on building and maintaining pressure. This system is more effective and is present in larger organisms such as humans.
The functions of the circulatory system generally include:
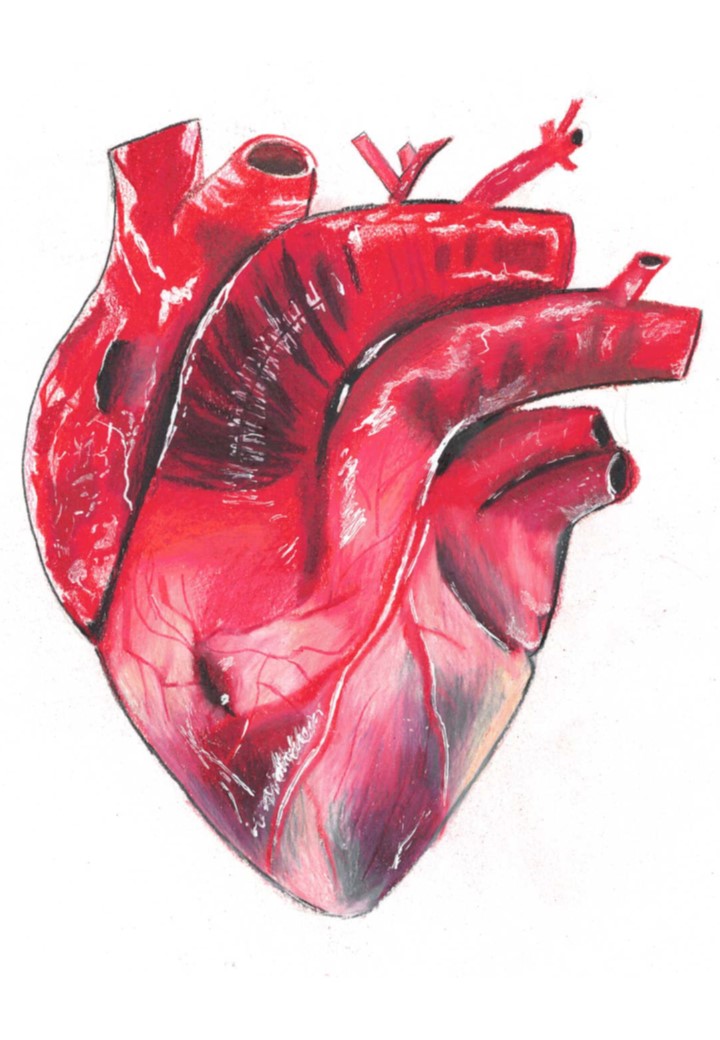
An illustration of the morphology of the heart.
The heart is a muscular organ located in the chest cavity and responsible for pumping blood to the lungs and to the rest of the body. It consists of two sides, the left and the right side, separated by a muscular wall called a Septum. The sides are named left and right in reference to the person facing the reader, so that the right side is actually on the left side of the webpage.
The right side pumps blood to the lungs and the left side pumps blood to the body. Each side is also split into two chambers for a total of 4 chambers. The upper chambers are called left and right atria, the lower chambers are called the Left and right ventricles. The ventricles are separated from the atria by valves, whose main purpose is to prevent backflow of blood.
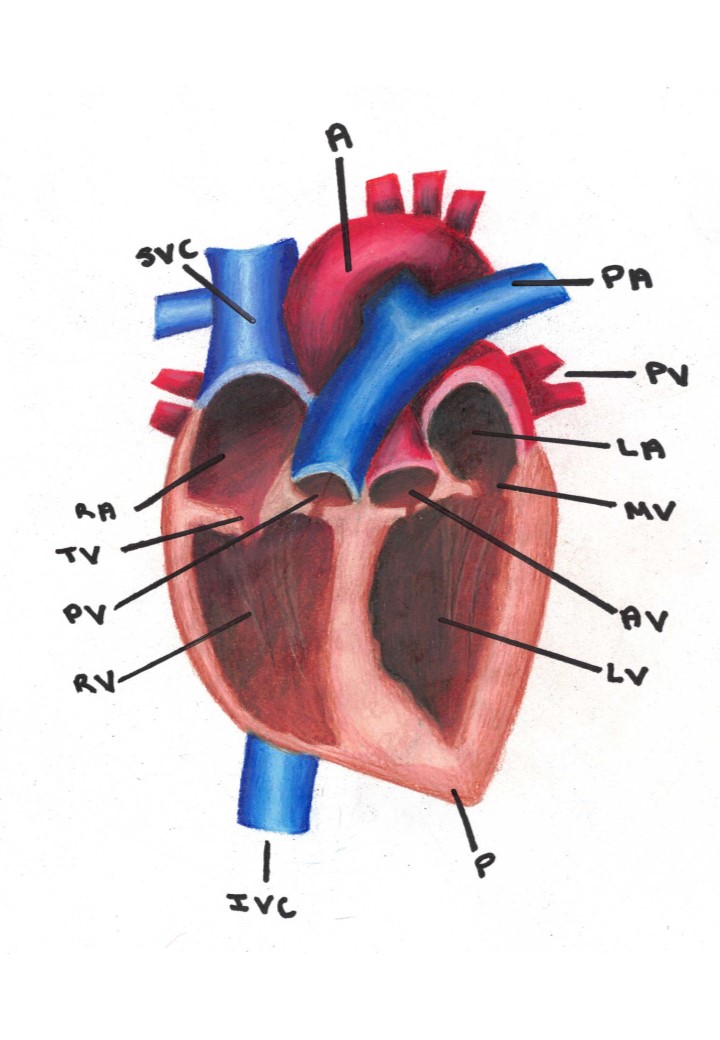
Parts of the heart. Legend: A: Aorta, PA: Pulmonary Artery, PV: Pulmonary Vein, LA: Left Atrium, MV: Mitral Valve, AV: Aortic Valve, LV: Left Ventricle, P: Pericardium, IVC: Inferior Vena Cava, RV: Right ventricle, PV: Pulmonary Vein, TV: Tricuspid Valve, RA: Right Atrium, SVC: Superior Vena Cava.
The circulatory system can be divided into 3 sections: Pulmonary (circulation in the lungs), coronary (circulation in the heart) and systemic (circulation to and from the rest of the body.
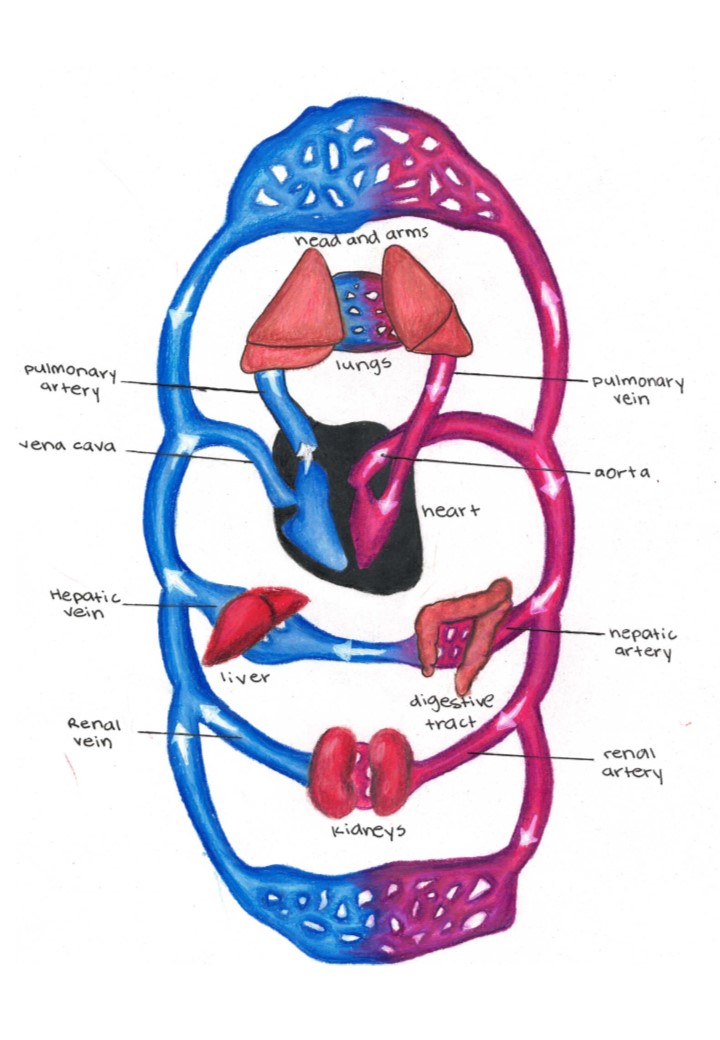
The main sections of the circulatory system.
Systemic Circulation: Involves 2 smaller systems Renal Circulation supplies and drains the kidneys, Hepatic Circulation - supplies and drains the liver and the digestive system. Some of the important blood vessels include: The Carotid Arteries and Jugular Veins supply and drain the head respectively, Brachial Artery and Brachial Vein supply and drain the arms respectively, Femoral artery and Femoral Vein supply and drain the legs respectively.
The heart is made up of cardiac muscles. A special type of muscles that can contract without receiving stimuli from the central nervous system. Cardiac muscles are made up of purkinje fibers.
The contraction mechanism of the heart involves:
The contraction of the heart is regulated by the autonomic nervous system. Sympathetic nerves are stimulated during stress causing the heart rate to increase. The Parasympathetic nerves are stimulated during times of non-stress returning the heart to a slow rate.

The contraction of the heart. (Source: Wikipedia, CC BY-SA 3.0)
Electrodes are placed on the body surface connected to a recording device. Electrical signals from heart are displayed on a screen or printed. The P wave represents the atrial contraction while the QRS wave represents ventricular contraction. ECGs can be used to detect some cardiac diseases especially under strenuous exercise.
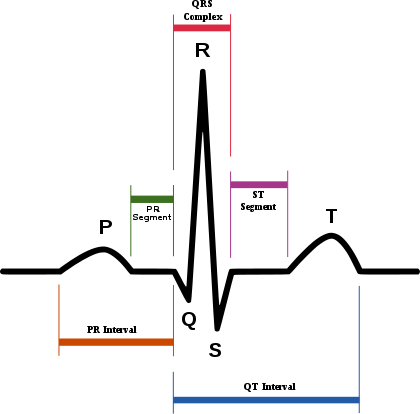
The electrocardiogram. (Source: Wikipedia, CC BY-SA 3.0)
In a mature person, the heart beats 70 - 75 times a minute. Each heartbeat can be split into 2 phases, Systole and Diastole. During Systole, the ventricles contract, while during Diastole, the ventricles relax. The two sides of the heart beat at the same time. Starting with the atria then the ventricles.
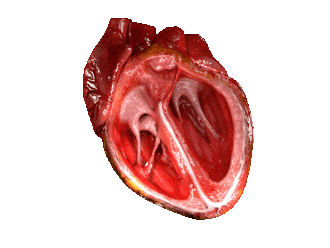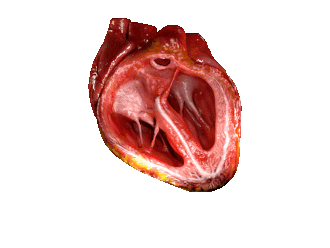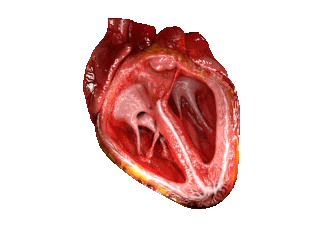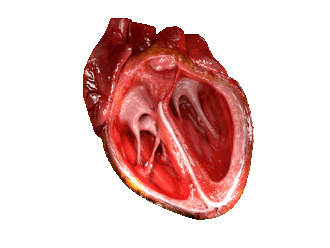
The cardiac cycle. (Source: Wikipedia, CC BY-SA 3.0)
The cycle starts with the heart relaxed; the two atria are filling with blood. Then the Atria Contract at the same time when the ventricles are relaxed. This is the Ventricular diastole causing the Ventricles to fill up. The blood passes through the AV valves as it enters the ventricles.
The cycle is followed by the contraction of the ventricles, called the Ventricular Systole. The AV valves close, and the semi-lunar valves open. The Right ventricle pumps blood through pulmonary artery to lungs, and the Left Ventricle pumps blood through the aorta to rest of body.
Systole (lubb) longest and loudest ventricles contract caused by AV valves closing.
Diastole (dubb) caused by semilunar valves closing ventricles relaxing.
Stroke Volume is The volume of blood per heart beat.
Heart Rate is The number of heart beats per minute.
The Cardiac Output is Stroke Vol. x Heart Rate. i.e. the volume of blood pumped by the heart in one minute.
Uses a sphygmomanometer to measure the arterial blood pressure. It is composed of two parts Systolic pressure, which is the larger number representing the pressure in artery when ventricles contract, and Diastolic pressure, which is the lower number representing the pressure in artery when ventricles relax. The normal blood pressure is about 120/80 and is and is considered too high if it exceeds 140/90 and too low if it's lower than 90/60. High blood pressure may be associated with several factors including high salt content, high epinephrine levels as in stress/freight, cancer, obesity etc. High blood pressure can cause heart attack, stroke, kidney damage etc. Low blood pressure is usually caused by low blood volume resulting from either bleeding, dehydration or severe anemia.
The regulation of blood pressure is a Negative Feedback mechanism. Baroreceptors located in the walls of aorta and carotid arteries detect blood pressure and send this signal to the Control Center i.e. the Medulla Oblongata in the brain. This center will initiate the response mechanisms such as vasoconstriction/vasodilation, or increasing/reducing heart rate etc.
An adult human is estimated to have about 100,000 km of blood vessels. Arranged end to end they would circle the Earth two and a half times.
All arteries carry blood away from the heart. They carry oxygenated blood except the pulmonary artery, which carries deoxygenated blood to the lungs. They have thick elastic walls, which recoil after a blood pulse passes through. The thick wall is necessary because blood in the arteries is at a high pressure. The Aorta is the biggest artery. Immediately after exiting the heart, it splits into two - Ascending and Descending Aorta, which supply the upper body and lower body respectively.
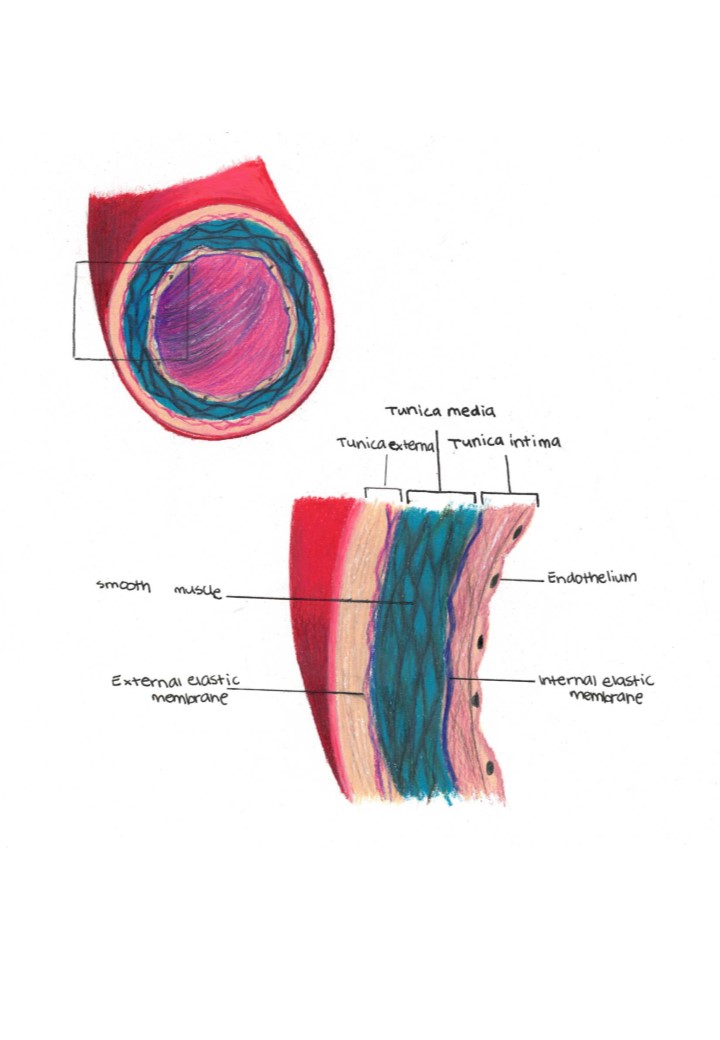
A cross-section illustrating the structure of an artery.
As the arteries move further away from the heart, they further subdivide into smaller sized arterioles.
Capillaries are very small blood vessels with a wall (endothelium) that is only one cell thick. These are the only blood vessels that allow for the exchange of water, gases, nutrients and wastes. Capillaries transfer material from blood to the fluid around cells (Interstitial fluid), and from the interstitial fluid into capillaries, through diffusion. Capillaries are so narrow that red blood cells can only pass through in a single file. Capillaries form a capillary bed, which is a group of many interconnected capillaries in one organ or section of an organ. As blood passes through the capillary bed, the nutrient concentration slowly reduce and the concentration of wastes increases.
on the other end of the capillary bed, as several capillaries merge, they form a venule. These contain blood that has been stripped of its nutrients and is laden with waste material such as carbon dioxide and urea.
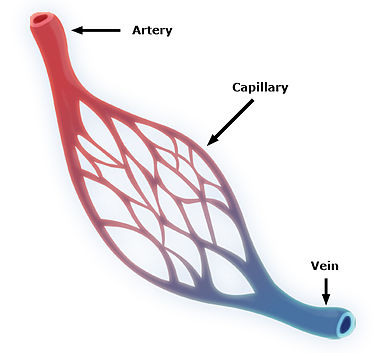
The structure of the capillary bed. (Source: Wikipedia, CC BY-SA 3.0)
Veins transport blood towards the heart. They are thin walled and the walls consist of smooth muscles that can contract and relax. They are a bit wobbly actually. Blood in the veins is at a low pressure and because blood is moving against gravity, it can tend to lug. To prevent backflow of blood, veins are supported by valves. Muscle movement during exercise also helps to move blood more effectively through the veins.
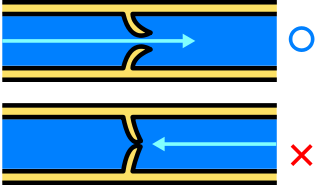
The venous valve and prevention of backflow. (Source: Wikipedia, CC BY-SA 3.0)
The portal venous system is a series of veins or venules that directly connect two capillary beds. Examples of such systems include the hepatic portal vein, which carries blood from the digestive system, filled with nutrients, into the liver, for metabolism and for detoxification.
Blood consists of three main components including Plasma (55%), Red Blood Cells - Erythrocytes (44%) and White Blood Cells and platelets (1%). Blood also contains proteins, sugars, minerals, vitamins and other small molecules in lower levels. The red blood cells are heaviest, followed by the white cells and then the least heavy is plasma.
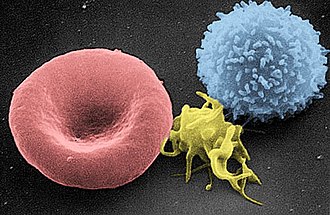
An electron micrograph of an erythrocyte (red blood cell), thrombocyte (platelet) and leucocyte (white blood cell). (Source: Wikipedia, CC BY-SA 3.0)
Red blood cells (RBCs / Erythrocytes) are produced in the red bone marrow through a process called Erythropoiesis. A mature male has about 5.5B RBCs in one ml of blood, while an adult female has about 4.5B. The difference is mostly attributed to blood loss during menses in females. RBCs are small, (8 microns in diameter), this allows them to pass through the tight capillary tubes. In most organisms, RBCs lack a nucleus, which is thought to increase the surface area available for the exchange of oxygen, however, because of the lack of a nucleus, red blood cells have a short life span of about 120 days, after which they are destroyed in a process that partially occurs in the liver. RBCs are biconcave in shape, which also increases their surface area for maximal gas exchange. It is this biconcave shape that gets messed up by sickle cell disease. Red blood cells are red due to the presence of Hemoglobin. hemoglobin is a complex between globin proteins and heme. Heme is rich in iron (gives blood an iron taste/smell) and plays a significant role in the transport of Oxygen.
There are several types of white blood cells, but can be classified into two major categories - Granulocytes and Lymphocytes. As the name suggests, granulocytes appear to contain granules when observed under a microscope. Granulocytes are produced in the red bone marrow. Adults have about 6000 of these cells in 1 ml of blood. They are large cells, about 25 microns. Granulocytes have a lifespan of only a few days. They function in the immune response. Some examples of granulocytes include Basophils, Neutrophils and Eosinophils.
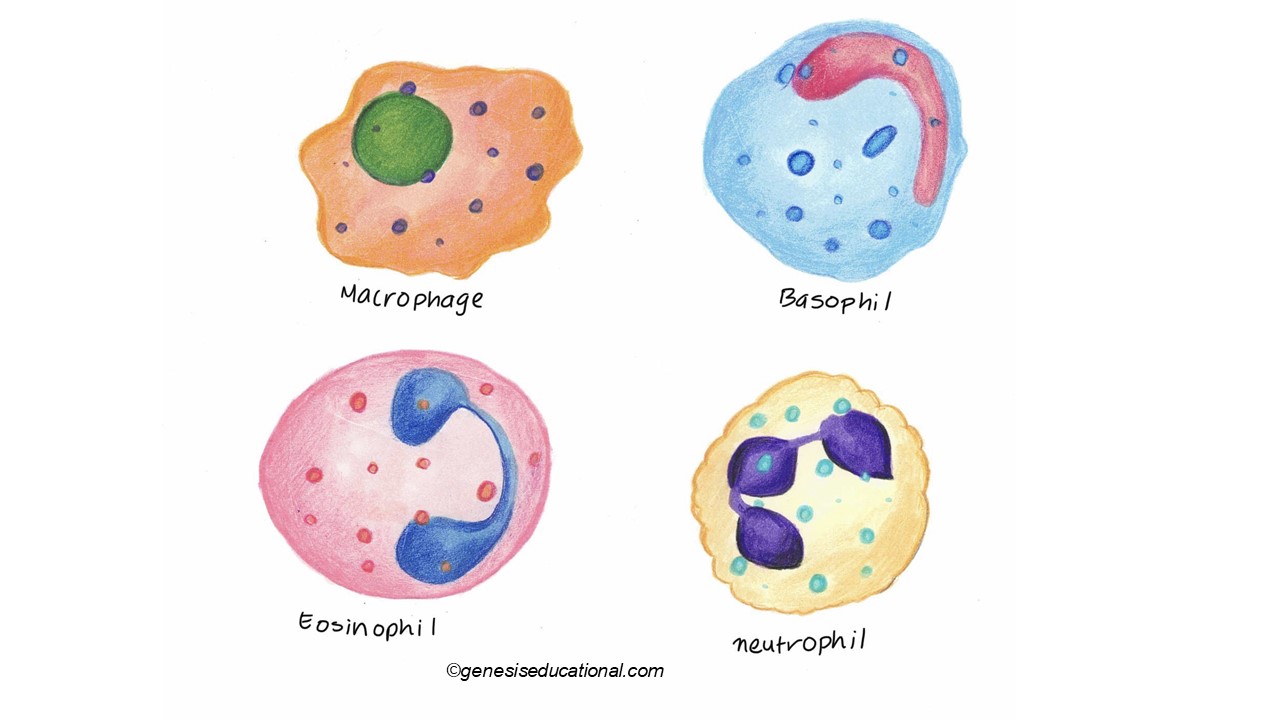
Lymphocytes on the other hand are produced in the red bone marrow and also the thymus. An adult has about 2000 lymphocytes in every milliliter of blood. Lymphocytes are also involved in the immune response, more especially in the synthesis and production of antibodies. Lymphocytes are categorized into B-Lymphocytes (from the bone marrow) and T -Lymphocytes, from the Thymus.
Platelets appear on the microscope, more like particles than cells, they are very small (2 microns) and are irregular in shape. They are produced in the red bone marrow and in lungs. An adult had about 250,000 platelets in every ml of blood. Platelets live up to 8 days and are involved in the blood clotting process.
When you remove all the cells from blood using a centrifuge, the liquid component that rises to the top of the tube is called plasma. About 90% of plasma is water. 7% is proteins including clotting proteins such as fibrinogen, globulin and albumin. Plasma also contains organic substances including urea and nutrients. Some of the inorganic ions present in plasma include calcium, chlorine, magnesium, potassium, sodium bicarbonates, phosphates and carbonates.
Lymphatic Circulatory System is a network of vessels, with associated glands or nodes that extends throughout the body. Lymph is a colorless or pale yellow fluid composed of interstitial fluid with a composition much like plasma. The lymph system uses one way valves and muscular contractions to produce fluid flow. Lymphatic Capillaries are close-ended vessels that transport fluids that ‘leak’ out of capillaries to bath the cells in one direction and back into the venous system. Lymph Nodes and glands that contain white blood cells called lymphocytes. Nodes are areas that trap and destroy bacteria, viruses and cancerous cells. These swell with increased lymphocytes and can be painful during infections.
Digestion is the mechanical and chemical breakdown of complex food into simpler compounds that can be absorbed and utilized by the body. Digestion begins in the mouth.
Major anatomical components of the digestive system
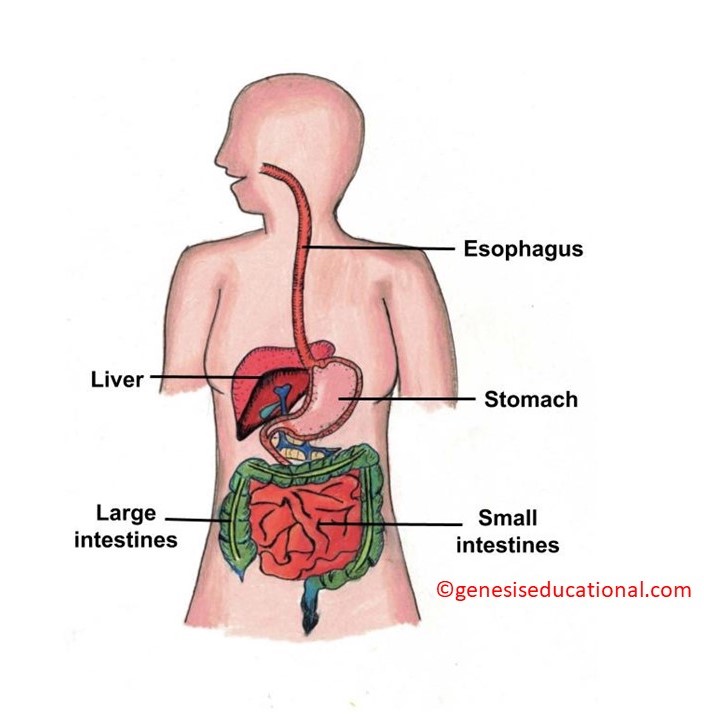
A general illustration of the digestive system.
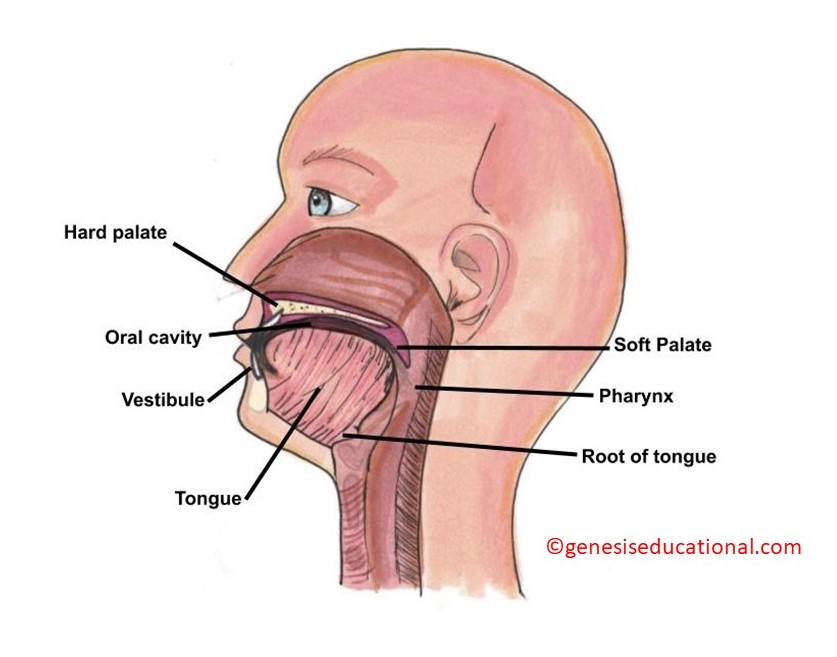
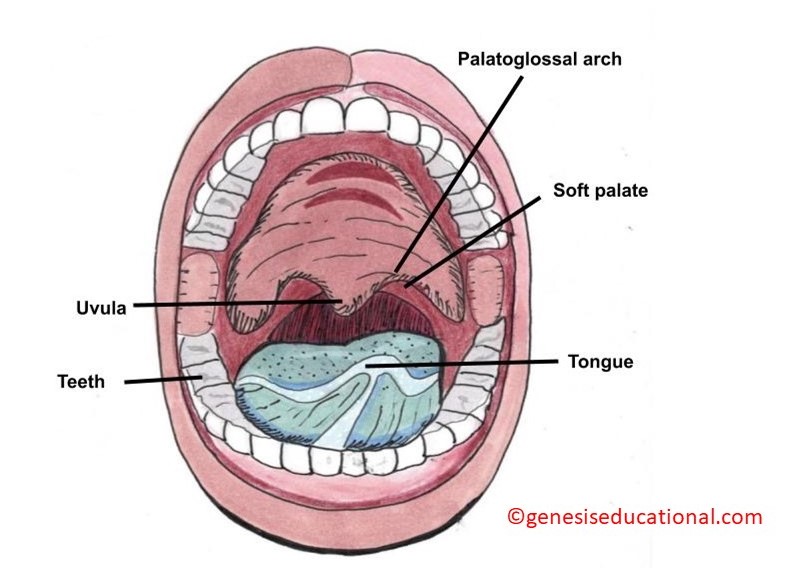
The structures of the oral cavity.
Location and types of salivary glands
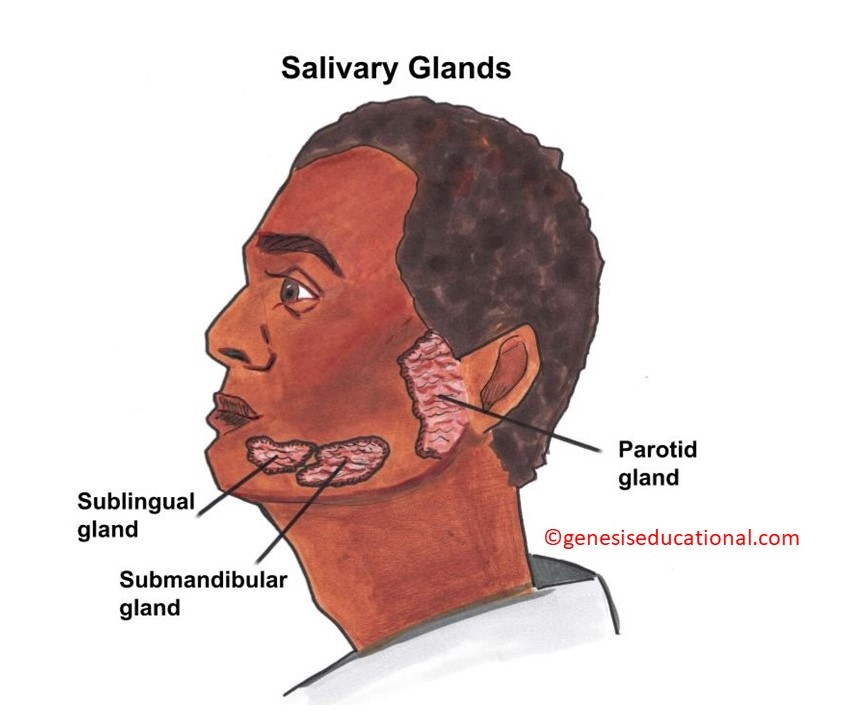
The 3 main salivary glands.
The bolus of food reaches the back part of the tongue and initiates the swallowing reflex. The pharynx is the common space for both the esophagus and the trachea. The epiglottis covers the trachea and prevents food from entering the trachea (aspiration).
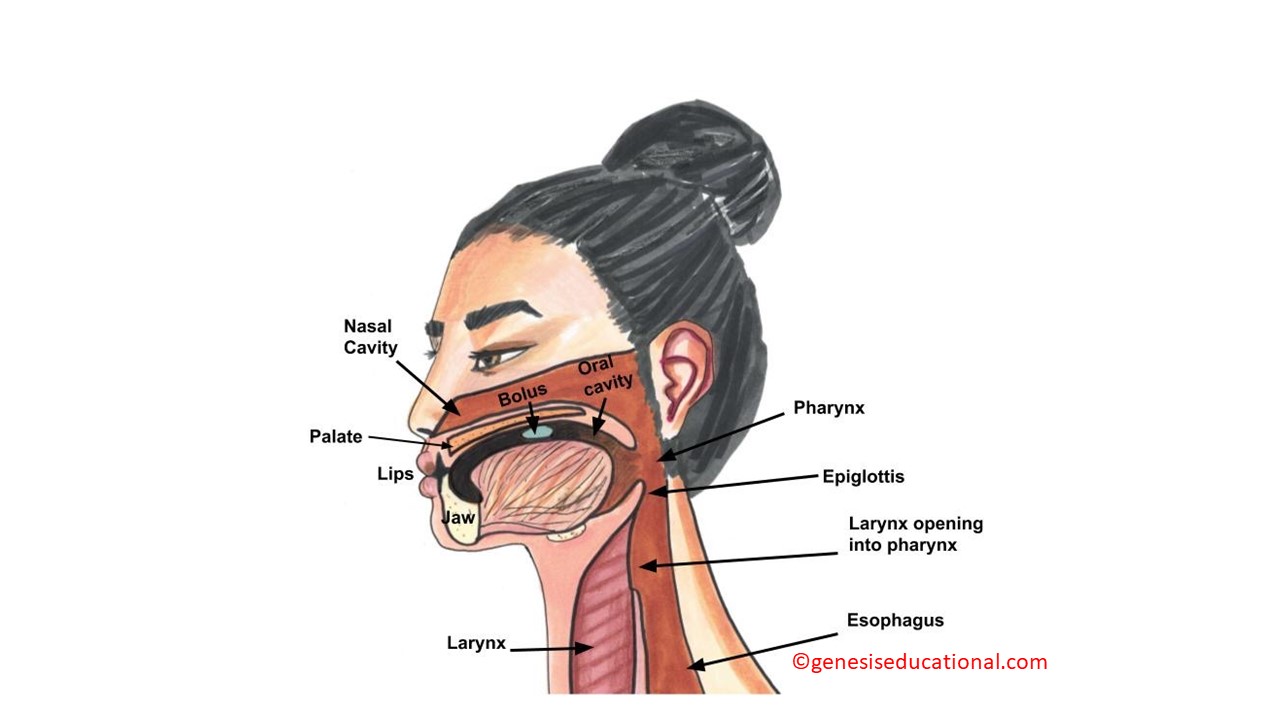
The anatomical structures associated with swallowing.
The esophagus is tube that connects the mouth to the stomach. It has smooth muscles that contract in waves creating the process called Peristalsis. Peristalsis is unidirectional (towards the stomach) unless the vomiting reflex has been initiated.
Peristalsis is an involuntary reflex, (not under human control). Reverse peristalsis (vomiting) may result in acid reflux where the acidic contents of the stomach enter the lower section of the esophagus causing irritation. Because peristalsis is autonomic and unidirectional, a food bolus will e moved towards the stomach regardless of the general body position. A person can swallow food even when he is standing upside down. The problem, however, is the functioning of the epiglottis, which blocks the trachea during swallowing. If the trachea is not well covered, then food particles may enter the trachea causing aspiration and triggering the coughing reflex.
The stomach is a sac / pouch like organ. It begins at the cardiac sphincter (gastro-esophageal sphincter) and ends at the pyloric sphincter, the gastro-duodenal sphincter. The stomach secretes gastric juices that contain Hydrochloric acid (HCL) and some enzymes.
The highly acidic environment is necessary to kill microorganisms in the food.
Enzyme pepsin results in the digestion of proteins. Pepsin is secreted by the stomach walls in form of Pepsinogen, an inactive form so that it does not digest the stomach wall. Pepsinogen is activated into pepsin when protein-rich food arrives in the stomach.
Chemical digestion is facilitated by the churning action of the stomach caused by contraction and relaxation of smooth muscles in the wall of the stomach. This churning action results in mixing of the partially digested food and gastric juice into a mixture called chyme.
Gastric emptying occurs within two to six hours after a meal. Chyme is released into the small intestines in small amounts at a time. The movement of chyme from the stomach into the small intestine is regulated by; (1) hormones, (2) stomach distension and (3) muscular reflexes that influence the pyloric sphincter (Gastro-duodenal sphincter).
Note that the stomach wall is not affected by the acid because it is lined by a thick layer of mucus.
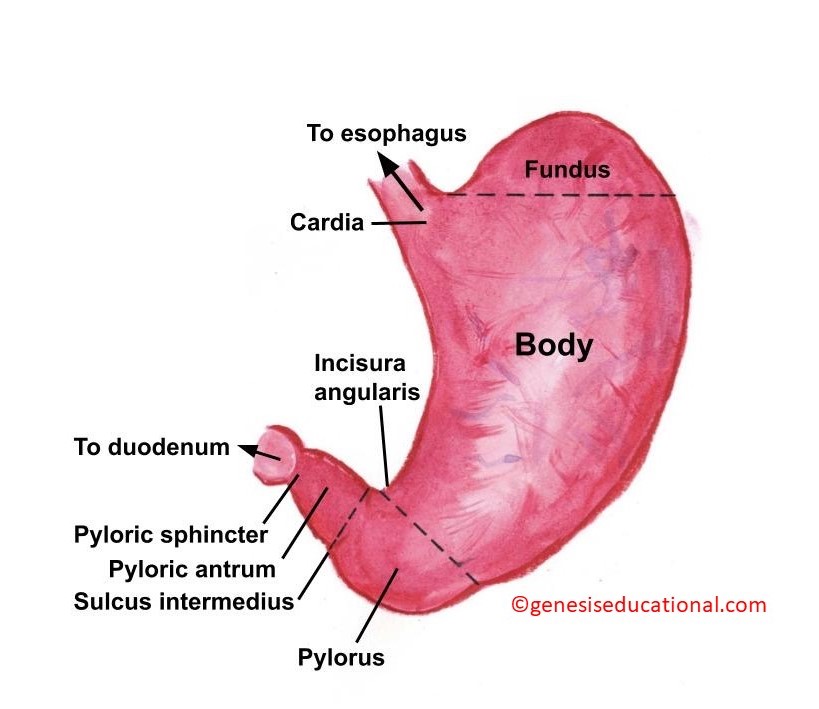
The parts of the stomach.
It’s a long tube-like organ with a highly folded surface containing finger-like projections called the villi. The top surface of each villus has many microscopic projections called microvilli.
Digestion of protein, fats, and carbohydrates is completed in the small intestines. The epithelial cells of these villi absorb nutrients from the digested food and release them to the bloodstream. The villi and microvilli, with their many folds, increase the surface area of the small intestine and increase absorption efficiency of the nutrients.
The human small intestine is over 6 m (19.6 ft) long and is divided into three parts: (1) duodenum, (2) jejunum and (3) ileum. The duodenum is separated from the stomach by the pyloric sphincter.
Pancreatic juices are alkaline with high bicarbonate levels to neutralize the acid from the stomach. This increases the pH creating the best environment for enzymes to function. Pancreatic juices also contain enzymes that digest proteins (pepsin and trypsin), fats (lipase) and carbohydrates (maltase). The end products of these enzymatic reactions include amino acids, fatty acids and glucose. These are all absorbed into the blood stream. Other nutrients that are absorbed in the small intestines include vitamins, minerals and other micronutrients.
Bile is produced in the liver and stored and concentrated in the gallbladder, and then released into the duodenum through the bile duct. Bile contains bile salts, which cause emulsification of lipids, (break down large droplets of lipids into smaller size) which increases the surface area and makes the lipids accessible to the water-soluble lipase enzymes.
The end products of digestion are absorbed in through the intestinal lining into the blood vessels, except fatty acids which are absorbed into the lacteal - that connects to the lymphatic system.
Intestinal smooth muscles also cause unidirectional peristalsis as food moves along the small intestines and into the large intestines. These peristaltic movements are regulated by the autonomic nervous system.
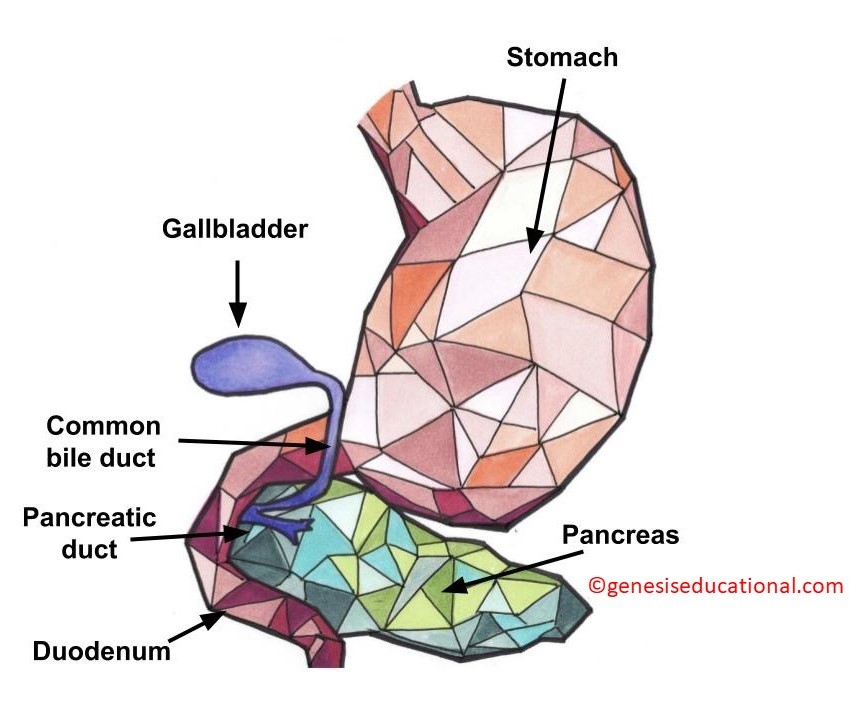
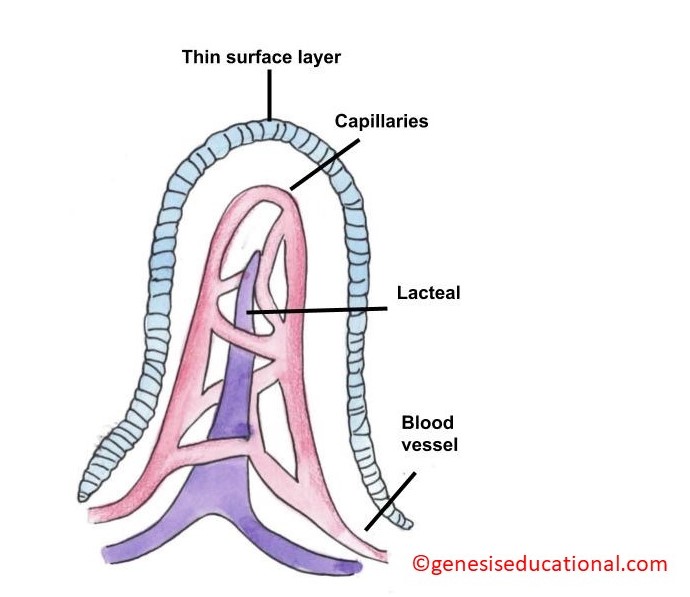
The structure of the duodenum (left) showing the location of the pancreatic and bile ducts. On the right is the structure of a villus (plural ~ villi).
Absorption of water occurs in the large intestines. The large intestines split into 3 parts; (1) cecum, (2) colon, and (3) rectum. In humans, the Colon divided into 3 sections; (1) Ascending colon, (2) Transverse colon and (3) Descending colon.
Involves 4 main processes:
Ingestion is basically the introduction of food into the mouth. Then mastication, which involves chewing of the food. You should be able to remember the meaning of terminologies such as mechanical and chemical breakdown of food, bolus and peristalsis.
Carbohydrates
Digestion begins in the mouth. Salivary amylase breaks down starch into maltose. Amylase cannot function in an acidic pH so no carbohydrate digestion occurs in the stomach. Pancreatic juices (released into the duodenum) contain pancreatic amylase, which continues the breakdown of starch and glycogen into maltose, a disaccharide. The disaccharides are broken down into monosaccharides by enzymes called maltase, sucrase and lactase.
Proteins
Most digestion occurs in the stomach and then in small intestines. Pepsin breaks down proteins into peptides. In the duodenum, the pancreatic juice contains – trypsin, elastase and chymotrypsin. These digest peptides at specific sites resulting in short chains of oligopeptides. Finally, peptidases (carboxypeptidase, dipeptidase, and aminopeptidase) play important roles in reducing the peptides to free amino acids.
Lipids
Lipid digestion begins in the stomach using lipase enzyme, but most of the lipid digestion occurs in the small intestines. In the duodenum, the gall bladder secretes bile salts. Bile causes emulsification of fats resulting in small globules (emulsion). This increases the surface area of lipids accessible to the lipase enzymes. Lipases break down the lipids into fatty acids and glycerides. These molecules can pass through the plasma membrane of the cell and enter the epithelial cells of the intestinal lining.
The bile salts surround long-chain fatty acids and monoglycerides forming tiny spheres called micelles. Micelles move to the small intestinal wall and the fatty acids separate from the micelles and diffuse through the villi. The long-chain fatty acids and monoglycerides recombine in the absorptive cells to form triglycerides, which aggregate into globules and become coated with proteins. These large spheres are called chylomicrons. Chylomicrons contain triglycerides, cholesterol, and other lipids and have proteins on their surface.
Elimination of undigested and waste material is the final step in digestion. The undigested food material enters the colon, where most of the water is reabsorbed. The colon is also home to the microflora called “intestinal flora” that aid in the digestion process. The semi-solid waste is moved through the colon by peristaltic movements of the smooth muscles and is stored in the rectum until defecation.
The anus has two sphincters, one is voluntary and the other is involuntary.
It is important for students to note the difference between excretion and secretion. Secretion being the release of biological molecules / substances such as enzymes and hormones to be used by the body for various functions. Secretion can also be the discharge of substances that require to be excreted. Excretion is the discharge of metabolic waste materials. This topic focuses a lot more on the discharge of excess water and nitrogen waste through the kidneys. This is because ammonia (the by-product of protein and nucleic acid breakdown is significantly toxic and needs to be eliminated fast from the body before it causes adverse physiological effects. The other major waste is carbon dioxide. This will be covered under the respiratory system. The kidneys are also responsible for several other metabolic waste products such as medicines, toxins, minerals etc.
Because waste is produced within every cell, blood is required to transport waste from the cells to the kidneys. Eventually, excretion must be in sync with Homeostasis. Substances that are available in the body in higher than biologically needed will be excreted, this includes water, which explains why people pee more frequently after drinking excessive fluids.
Osmoregulation, one of the homeostatic processes, is the regulation of water and salt concentration in the body.
Amino acid deamination results in the formation of Ammonia. This is a highly toxic compound that cannot be allowed to accumulate in the body. Among other effects, Ammonia quickly results in increasing the body's pH making it more basic, which can affect several physiological functions. Ammonia is converted into less toxic uric acid and urea.
Uric acid is produced and excreted by birds. It is not soluble and is excreted as a white paste ensuring there is minimal water loss.
Urea is produced in mammals, in the liver from the deamination of amino acids. Urea is soluble in water and is excreted mixed with water and other substances in what is called urine.
The Human excretory system is made up of two kidneys – produce urine by filtering the blood, two ureters – take urine from kidneys to the bladder, the urinary bladder – stores urine and Urethra – carries urine to the environment.
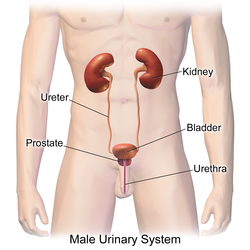
The structures associated with the male urinary system (Source: Wikipedia-CC BY-SA 3.0)
The kidney has three distinct regions:
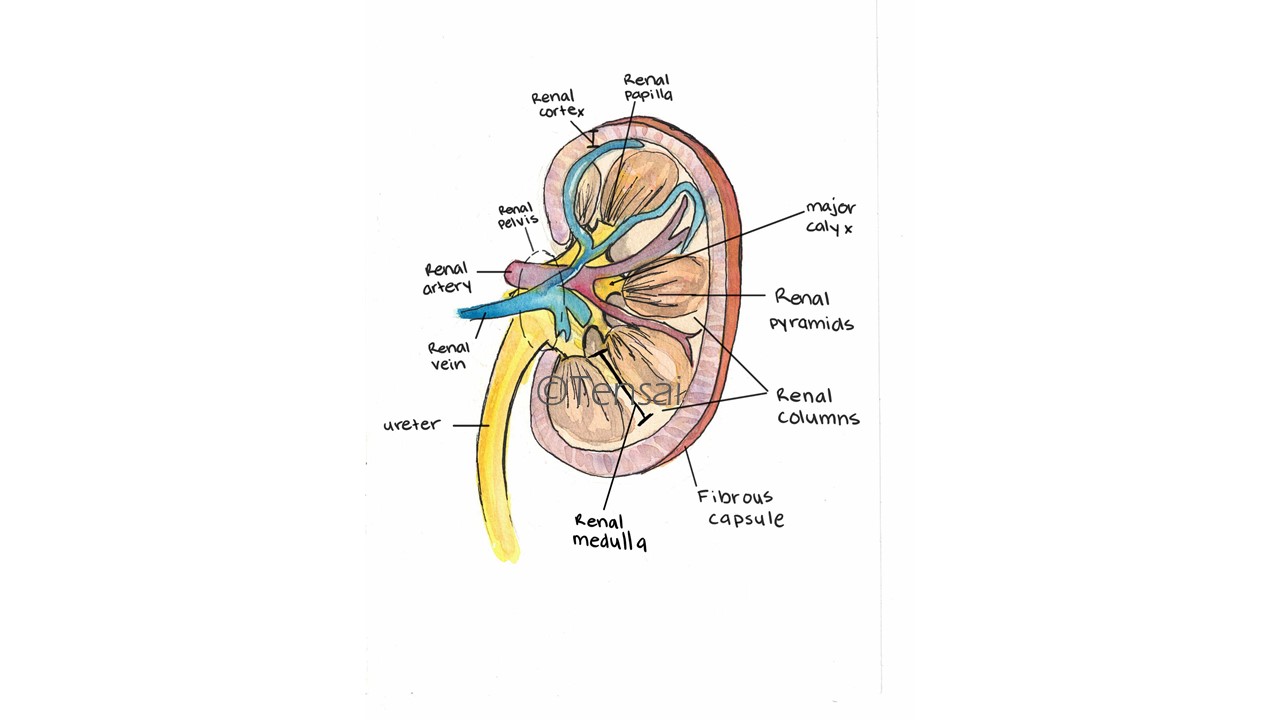
A detailed structure of the kidney.
The basic structural and functional unit of the kidney is the Nephron. Each kidney has approximately one million nephrons.
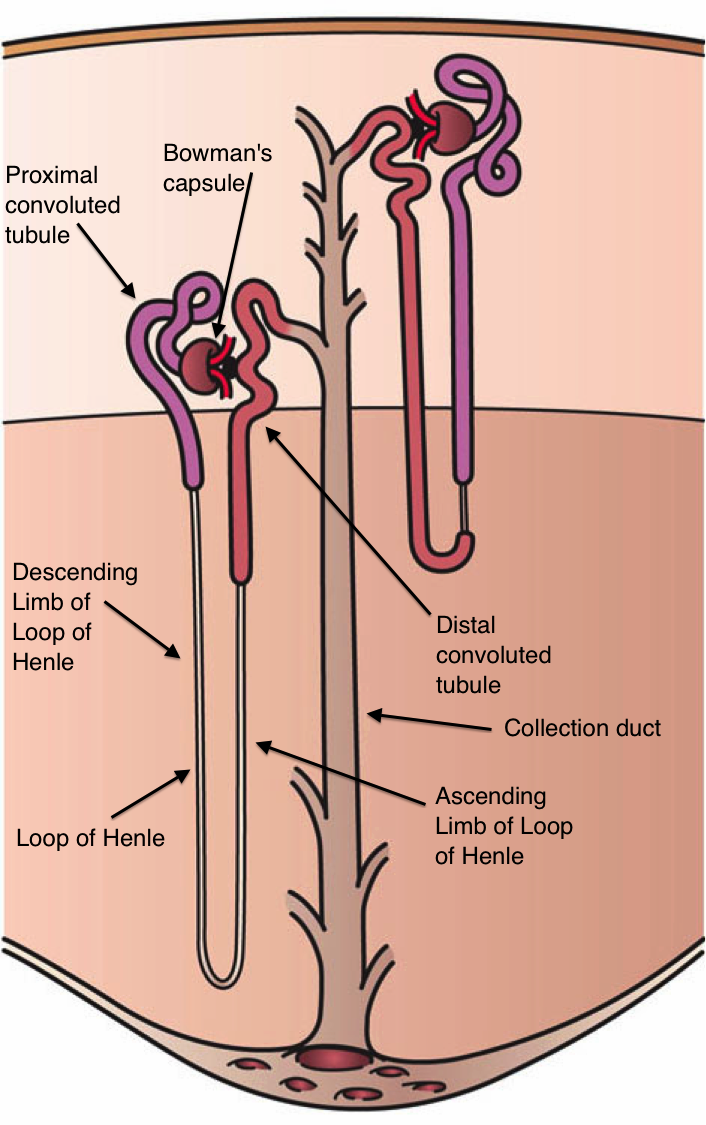
The parts of a nephron. (Source: Wikipedia-CC BY-SA 3.0)
The Bowman's Capsule: Consists of a double walled chamber supplied by a network of blood vessels (capillaries). The blood vessel that brings blood into the Bowman's capsule is called the Afferent arteriole, while the vessel that takes blood outside the capsule is called the Efferent arteriole. The Afferent arteriole is larger/wider than the efferent arteriole so more blood is supplied to the capsule than the amount leaving. This creates increased pressure (about 4 times higher) in the capsule, which results in ultrafiltration where plasma enters the glomerulus. This is called glomerular filtrate.
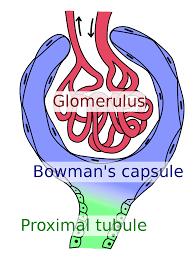
The structure of the Bowman's capsule with the afferent arteriole larger than the efferent. (Source: Wikipedia-CC BY-SA 3.0)
Proximal tubule: The proximal tubule is the section immediately after the glomerulus. Here, several substances (such as glucose, sodium and amino acids) are reabsorbed into blood through active transport.
Loop of Henle: It looks like a long hairpin structure. Here, some of the remaining water and salt in the filtrate will be reabsorbed back into the blood. The loop of Henle is located in the kidney's medulla, which is relatively hypertonic allowing for the movement of water.
Distal Convoluted tubules and Collecting ducts: This is the twisted section of the tubule immediately after the Loop of Henle. Here, more water reabsorption occurs. The antidiuretic hormone (ADH) is necessary to facilitate the reabsorption of water at this site. (Diuresis is a condition where too much water is present in urine, ADH is antidiuretic). The amounts of substances are reabsorbed into blood in precise amounts depending on the homeostatic regulation. Several nephrons connect to the same collecting duct, which then drains into the renal pelvis.
Occurs at the junction between the glomerulus and the porous wall of the Bowman’s capsule. The afferent arteriole is larger than the efferent arteriole; pressure builds up inside the glomerular capillary network. Only Fluid and dissolved materials (nutrients, wastes, ions) in the blood plasma pass from the glomerulus into the Bowman’s capsule. Red blood cells, plasma proteins and platelets are too large to pass through the wall of the capillary and therefore remain within the capillaries. The fluid that is filtered is called the Nephritic filtrate or Glomerular filtrate.
This is the process where important substances are reabsorbed back into the blood circulation. It starts from the proximal tubule to the collecting ducts. Between 85% - 99% of glomerular filtrate is taken back to the blood, depending on how much water and salt has been consumed, or needs to be retained. The efferent arteriole feeds into the vasa recta, a capillary network that surrounds the tubules. Reabsorbed substances enter this capillary network and eventually join the renal vein.
A more selective, precisely regulated reabsorption occurs in the distal tubules Additional quantities of salts and water may be reabsorbed. The exact amount of each substance reclaimed occurs in the distal tubules. Excess is excreted in urine e.g. glucose and diabetes
Hydrogen: The secretion of hydrogen ions help to regulate the pH of the blood. It is coupled to the reabsorption of sodium into the blood.
Potassium: High levels of potassium in the blood affect nervous function and affect muscle contraction. You can see the role of potassium under the nervous system topic. Because of this, the body has to ensure there is no accumulation of Potassium in blood.
Other substances that are secreted in the distal tubules are medications (such as penicillin), creatine (a by-product of protein breakdown) and other minerals/salts.
The urinary bladder stores urine before it can be eliminated to the environment. Urine flows from the kidneys, through the ureters and drips into the bladder. When the bladder is full, the pressure on its wall results in micturition/urination.
Is the actual elimination of urine through the urethra into the environment.
Hormonal regulation of excretion: Students are encouraged to review the Endocrine system, with specific emphasis on the hormones Antidiuretic hormone (ADH) and Aldosterone.
Should be differentiated from diabetes mellitus, the one caused by high sugar levels in blood. Diabetes Insipidus is a disorder in which the body does not produce sufficient ADH, so there is no reabsorption of water resulting in large volumes of dilute urine (diuresis). This could result in dehydration.
Hemodialysis means "cleaning the blood." In hemodialysis, the blood is circulated through an artificial kidney (machine), which has two spaces separated by a thin membrane. Blood passes on one side of the membrane and dialysis fluid passes on the other. The wastes and excess water pass from the blood through the membrane into the dialysis fluid, which is then discarded. The cleaned blood is returned to the bloodstream.
Uroliths for from the crystallization of salts in urine before it exits the kidneys. They vary in size from small grain-of-sand size to larger bead-like size. Most pass out of the body without help from a doctor but sometimes a kidney stone ma get stuck in the urinary tract, block the flow of urine and cause intense pain. Uroliths may also result in blood in urine or urine that smells bad or looks cloudy. Sometimes the patient develops a burning sensation during urination.
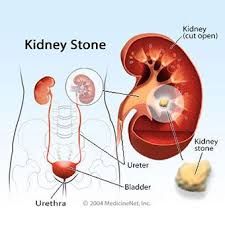
An illustration of the urinary bladder, ureters, kidneys and a kidney stone. (Source: https://www.medicinenet.com/kidney_stones/article.htm 2004; no copyright infringement intended.)
A muscle is a contractile tissue found in animals that acts by contracting and relaxing, and by doing these, will result in movement.
There are three kinds of muscle: skeletal (striated), smooth (visceral) and cardiac. Each type of muscle is specialized for its specific function.
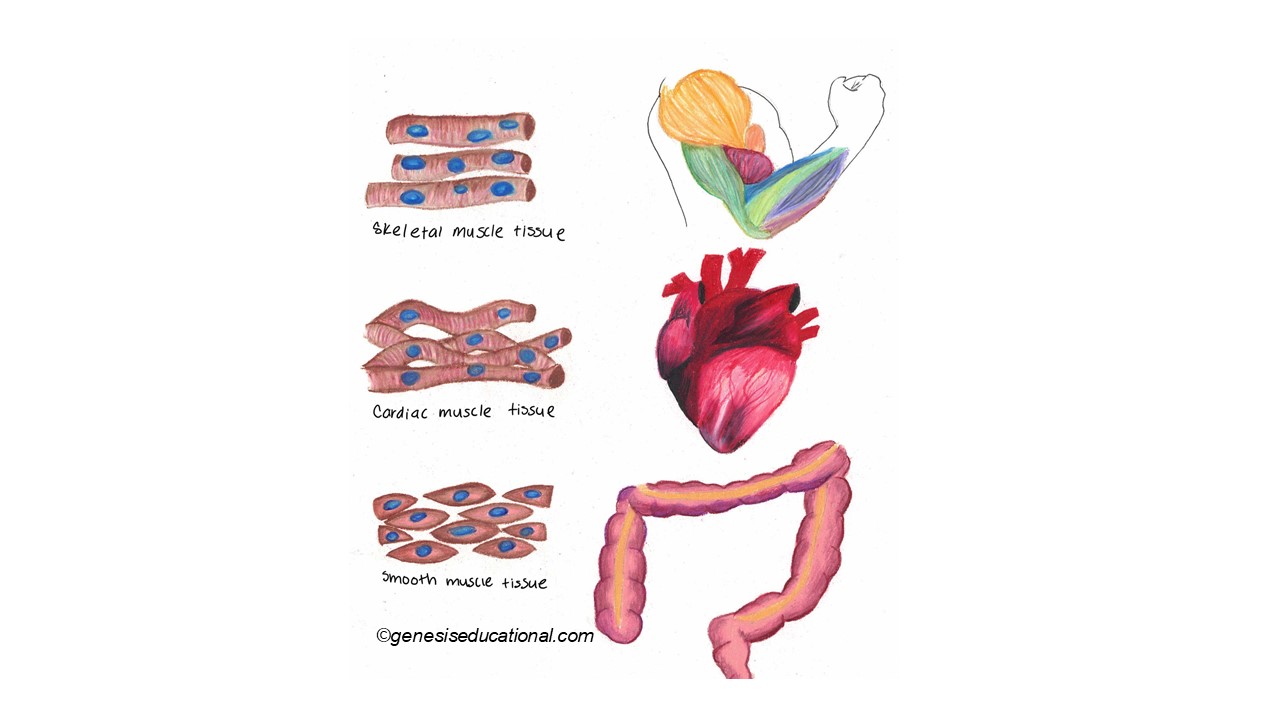
Three types of muscles. (Source: Wikipedia-CC BY-SA 3.0)
Muscles work by contracting (shortening) or relaxing (lengthening). Many skeletal muscles are arranged in antagonistic pairs that work against each other to produce movement involving a joint. For example the Biceps and the Triceps are antagonistic to each other.
Each skeletal muscle is composed of parallel bundles and each bundle is composed of parallel units called muscle fibers. Each fiber is actually a functional single cell containing many nuclei. Some of these fibers are extremely long single muscle cells. For example, the muscle fibers in the leg may be half a meter in length. Muscle fibers are enclosed within a membrane called sarcolemma, which is a delicate sheath surrounding muscle fibers.
Within the muscle fibers are tiny myofilaments bundled together.
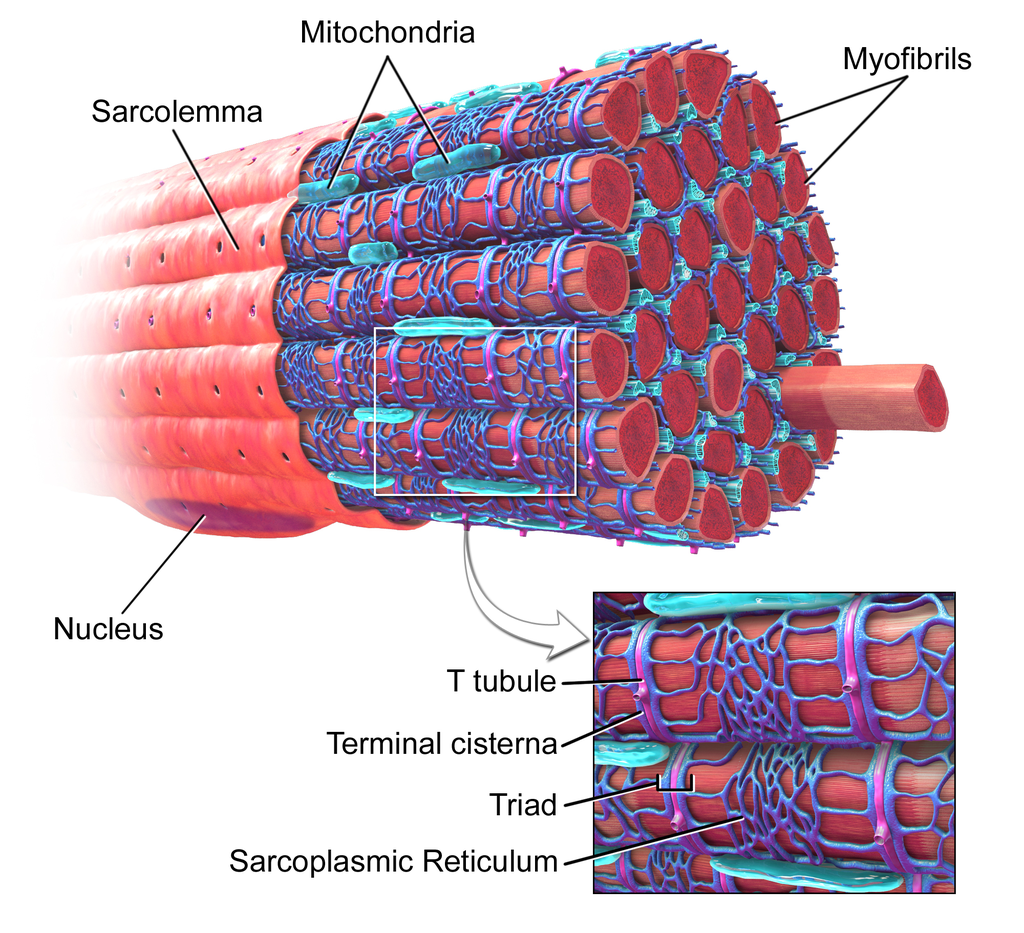
Muscle structure. (Source: Wikipedia-CC BY-SA 3.0)
Skeletal muscles are voluntary muscles anchored on both ends by tendons onto adjacent bones and they function in callusing movement/locomotion. An average adult male is made up of 42% of skeletal muscle and an average adult female is made up of 36% (as a percentage of body mass).
Muscle fibers are composed of tiny myofilaments bundled together. Each muscle fiber has two types of filaments i.e. thin filaments composed of the protein actin, and thick filaments composed of the protein myosin. The actin and myosin fibers overlap and create the striations that are characteristic of skeletal muscle.
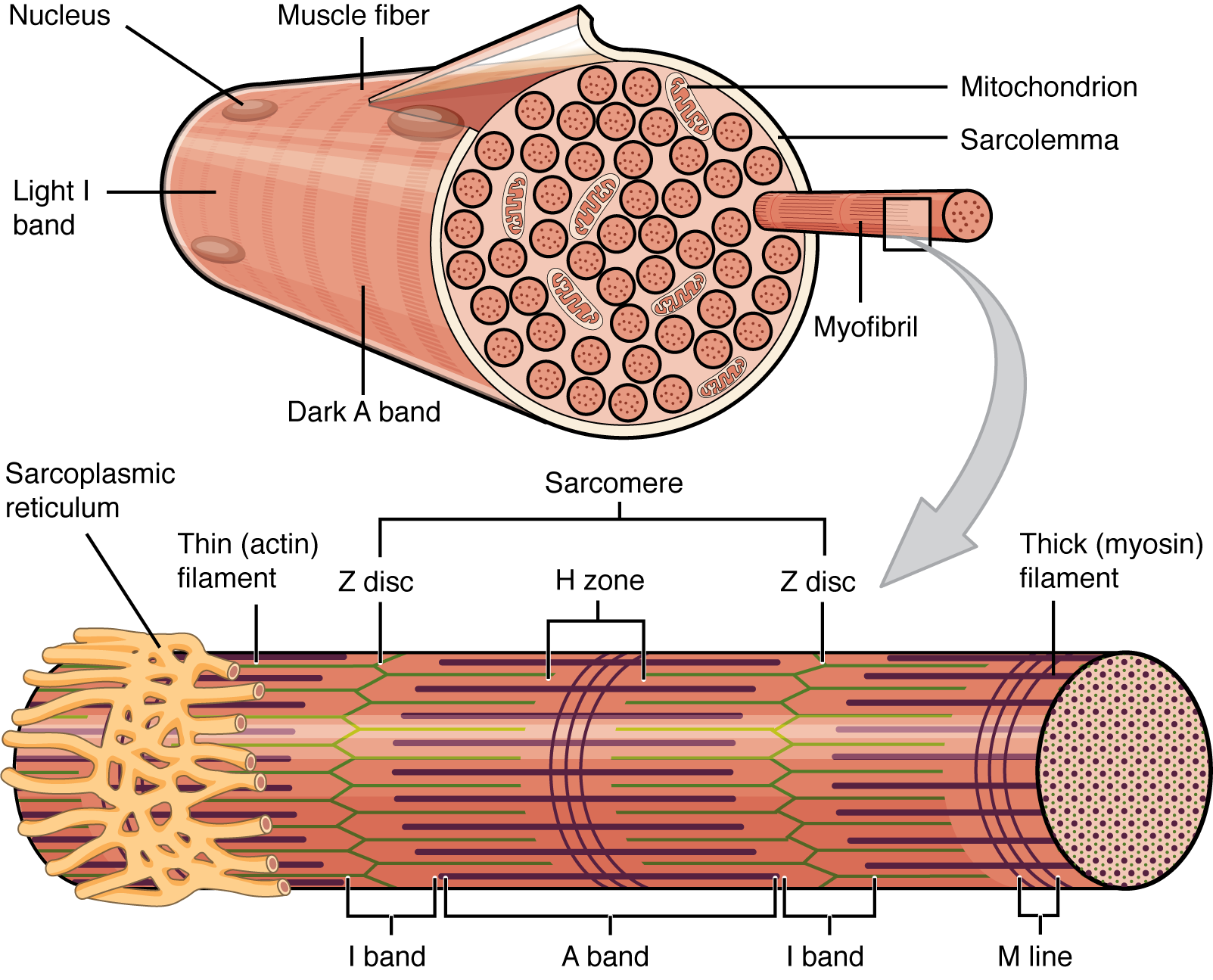
Illustration of skeletal muscle striations. (Source: open.oregonstate.education)
The contraction process of the muscle involves the sliding action of thin actin filaments over the thick myosin filaments. This process utilizes ATP.
Type I: are associated with slow muscle twitch. As a result, they use ATP slowly but are more efficient. Because of this they are more dominant among long distance runner or in wings of birds. They are rich in mitochondria and myoglobin, therefore they tend to be more red in color.
Type IIa and Type IIx: are fast twitch muscles. They break down ATP faster but with low efficiency. They are found in sprinters and animals that run very fast but for short distances. They tend to be pale in color evidence of less myoglobin. Because of the speed, they undergo anaerobic respiration so they can only perform for a limited time before they experience extreme pain from fatigue.
Cells obtain energy through the oxidation of organic compounds. The most abundant oxidizing agent on Earth is oxygen. As such, humans need oxygen to survive. Any prolonged absence of oxygen will result in death. The goal of the respiratory system is to provide the body with adequate amounts of oxygen needed for survival.
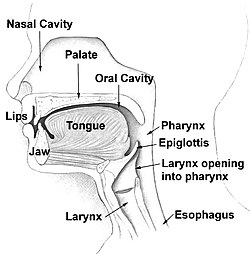
The upper respiratory system. (Source: Wikipedia-CC BY-SA 3.0)
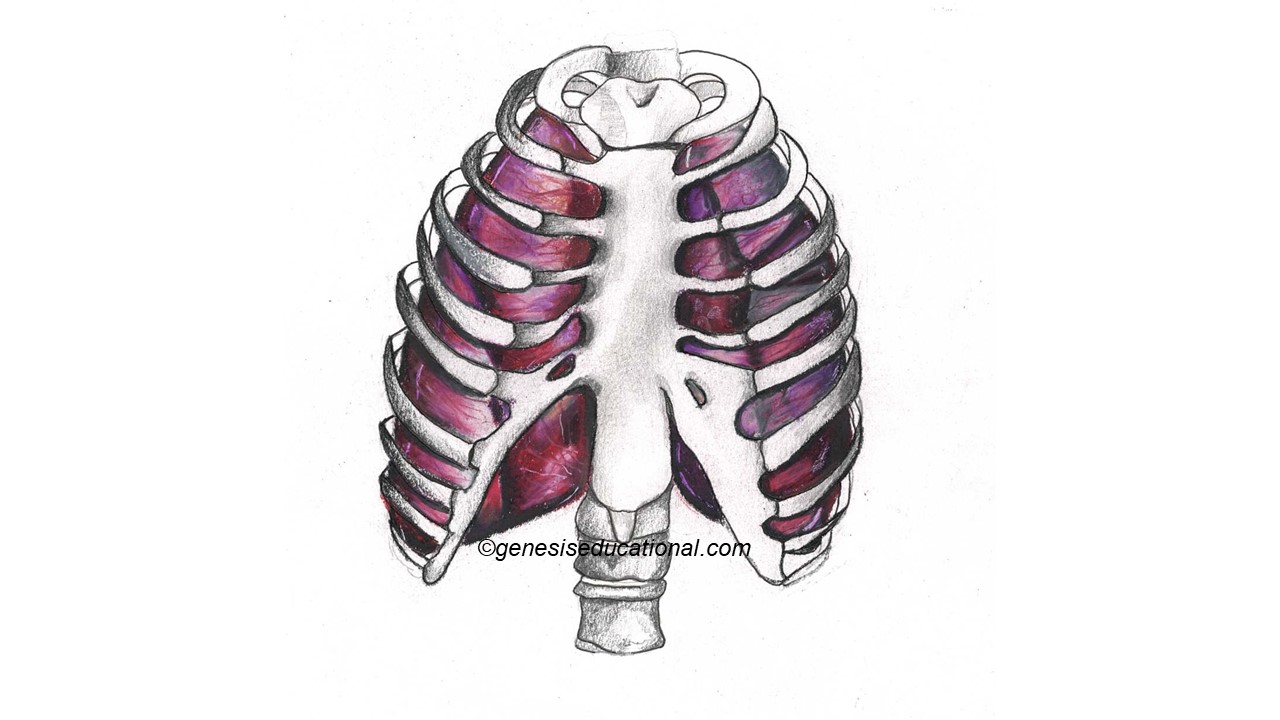
The rib cage
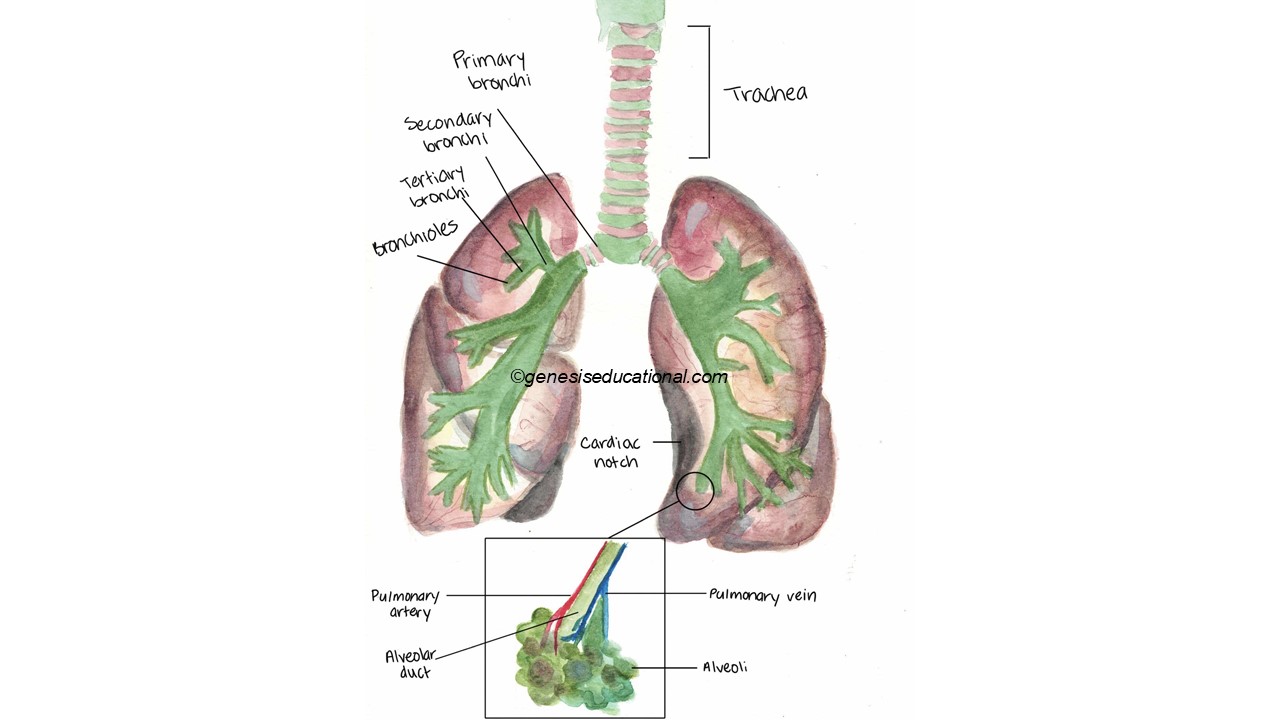
The structures associated with the respiratory system.
The concentration of carbon dioxide is important. The breathing center in the brain is located in the Medulla Oblongata. It controls the rate and depth of breathing. The medulla is sensitive to CO2 levels in the blood. When CO2 level is too high the medulla sends signals to the diaphragm and intercostal muscles to increase activity- both contract and result in inhalation. Once CO2 levels drop to normal range, the signal from the medulla stops.
The concentration of oxygen normally does not directly affect breathing rates. However, when oxygen levels are too low, signals from the aorta can increase breathing levels.
1. Holding Your Breath: When you hold your breath, carbon dioxide levels increase. As a result, when you allow breathing to occur, it will occur at a faster rate and deeper than usual.
2. Exercise: Exercise results in accumulation of carbon dioxide, which, as expected, results in increased respiratory rate and depth.
3. High Altitude: As the altitude increases, the concentration of oxygen in the atmosphere reduces. The oxygen receptors in the aorta will increase both the breathing and circulatory rate. Exposure to high altitudes over prolonged periods of time result in thickening of the left ventricular wall, due to increased demand for systemic blood circulation. This is called high altitude disease.
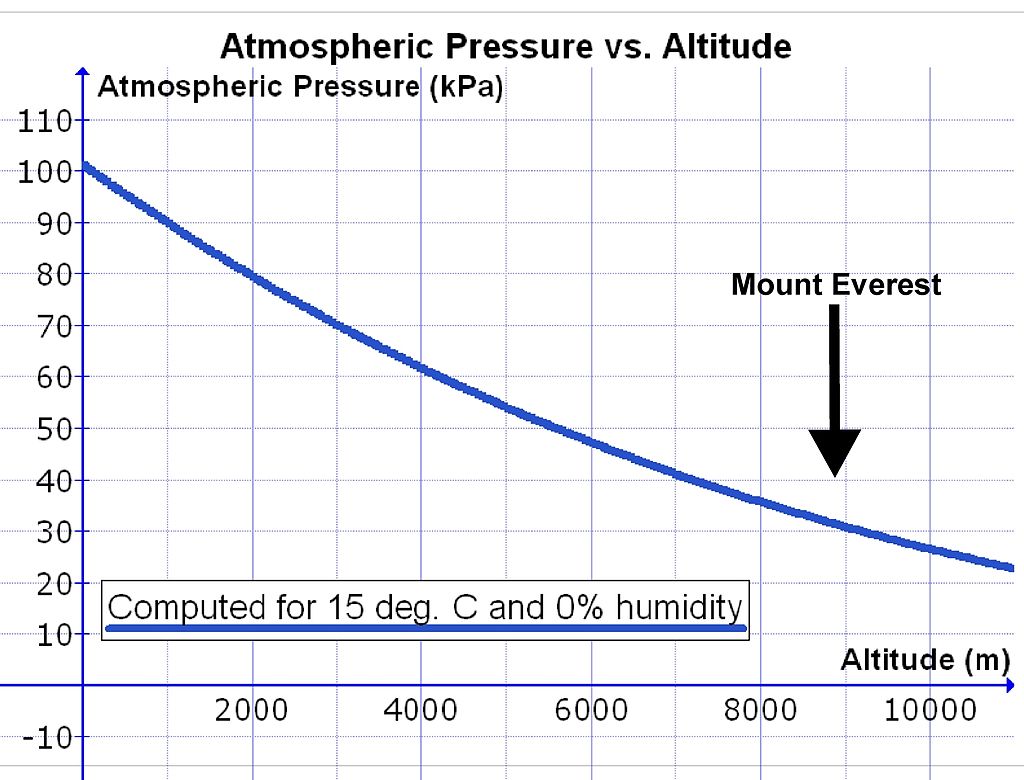
The graph shows the relationship between altitude and atmospheric air pressure. (Source: Wikipedia-CC BY-SA 3.0)
4. Carbon Monoxide: Carbon monoxide (CO) binds to hemoglobin to form carboxyhemoglobin and acts as a competitive inhibitor in the red blood cell blocking carbon dioxide and oxygen. The affinity of Hemoglobin to carbon monoxide is about 200 times higher than Hemoglobin to oxygen. This makes the hemoglobin unavailable for oxygen and carbon dioxide. Theoretically, the accumulation of carbon dioxide would result in increased respiratory rate, but the absence of oxygen is more detrimental resulting is possible death from anoxia.
1. Hyperventilation: When a person hyperventilates, the carbon dioxide levels are reduced. This reduces the respiratory rate and someone is able to hold his or her breath for a longer time.
Oxygen Transport
Hemoglobin transports about 97% of the oxygen. The remaining 3% is transported in plasma. The hemoglobin molecule is composed of 4 peptide (globin) chains with an iron (heme) center. Hemoglobin that has oxygen attached to it is called oxyhemoglobin. The hemoglobin that is free of oxygen is called deoxyhemoglobin. Oxygen enters and leaves the hemoglobin molecule through diffusion.
Carbon Dioxide Transport
As an adaptation to ensure increased chances of survival by effective elimination of waste, material, carbon dioxide can be transported in blood in several ways. About 64% of CO2 is transported in plasma as bicarbonate ions. About 27% of CO2 combines with hemoglobin to form carbaminohemoglobin. The remaining, approximately 9% of CO2 is dissolved in plasma.
Carbon dioxide continuously diffuses from cells, such as muscles, into blood. Some of the carbon dioxide dissolves with water in plasma to form carbonic acid, which then breaks down into H+ and bicarbonate ions. The H+ is combined with hemoglobin to prevent drastic pH changes, while the bicarbonate ions stay in the plasma. When this blood reaches lungs, O2 will combine with hemoglobin displacing H H+ into plasma. The H+ recombines with bicarbonate ion producing water and carbon dioxide, which diffuses into alveoli to be exhaled.
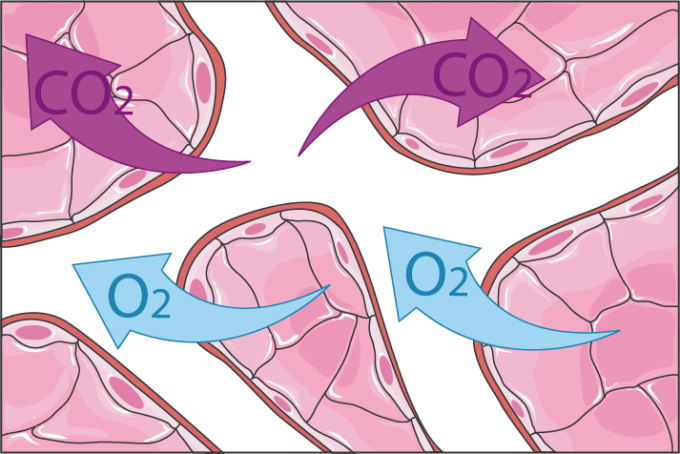
The exchange of gases between the alveoli and blood capillaries. (Source: Wikipedia-CC BY-SA 3.0)
In the lungs alveoli (singular – alveolus) there is a higher concentration of oxygen compared to the concentration of oxygen in the blood. However, there is a lower concentration of carbon dioxide in the alveoli than the concentration of carbon dioxide in the blood. This concentration gradient results in the movement of oxygen from the alveoli air into the capillary network where it attaches to hemoglobin. Carbon dioxide moves from the blood across the alveoli and into the alveoli.
Inhalation
Exhalation
Below is a summary illustration of the production of blood cells by the bone marrow and thymus.
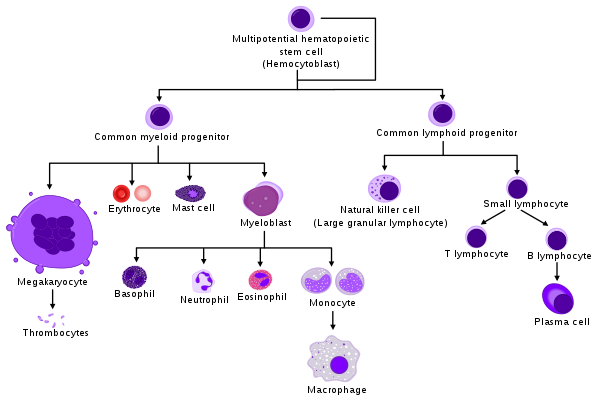
Hematopoietic processes for various blood cells. (Source: Wikipedia, CC BY-SA 3.0)
The Circulatory, Lymphatic and Immune responses work closely together. Specifically, the Immune System is designed to fight infections (caused by pathogens) and other particles that are deemed 'foreign' by the body (such as allergens). A pathogen is an organism that can cause harm allowed to live and multiply in/on the body. There are four main types of pathogens:
Blood clotting can occur either intrinsically or extrinsically. Extrinsic factors involve injury what causes a destruction of a blood vessel. Intrinsic and extrinsic pathways are too complicated for this level of biology. What you need to remember are the steps that are common in both extrinsic and intrinsic pathways.
The simplified process involves the conversion of prothrombin to thrombin by other clotting factors. Thrombin functions, among other functions, to convert fibrinogen to fibrin. Fibrin forms covalent bonds that crosslink to form a mesh that plugs the injury and stops the bleeding.
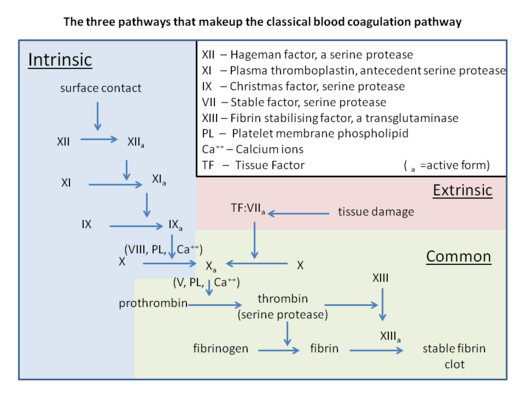
Blood clotting process. Please note that high School students need to focus on the section labelled 'common' only. (Source: Wikipedia, CC BY-SA 3.0)
The first line of defense can be looked at as preventing the entry of pathogens into the body. Most barriers that protect the internal body from the environment will act as first like of defense. These include:
The second line of defense can be categorized into two main categories: Specific and Non Specific. Non-specific response is a cell mediated response involving phagocytic cells engulfing pathogens. Neutrophils target mostly bacteria and fungi. Eosinophils target parasites. Basophils are involved more in allergic reactions. Macrophages can engulf all kinds of pathogens.

Specific immune responses are mediated by Antibodies. Pathogens cause disease by the presence of Antigens, which are proteins located on the surface of pathogens. Antibodies are molecules that are produced by lymphocytes in response to the presence of specific antigens; therefore, an antigen will neutralize the specific antigen it was produced for.
Memory B and T lymphocytes are lymphocytes that retain a memory of the antigen structure for a prolonged period, so that in future if the individual is infected by the same antigen, the memory B and T cells will recognize it and initiate faster antibody production. Suppressor T cells are meant to slow down the immune response especially when the antigens have been eradicated.
Vaccination uses either a weakened pathogen or a part of the pathogen that causes an immune response in the host. Memory cells produced through vaccination remain in the blood for a long time therefore, a vaccinated person responds better/faster when exposed to the antigen a second time.
This a group of conditions that occur when T – cells or antibodies mistakenly attack the body’s own cells. Examples include:
Rheumatoid Arthritis: A chronic disorder caused by the immune system attacking the body’s joints resulting in inflammation and damage of cartilage, tendons and bone.
An allergy is an exaggerated immune response to materials that are supposed to be harmless.
You can access Tensai High School Biology revision questions HERE